Why Surgeons Feel So Fatigued. These 700 Gloves May Have The AnswerWhy Surgeons Feel So Fatigued. These 700 Gloves May Have The Answer
As a surgeon, I know firsthand the grueling demands of the job. The long hours, back-to-back surgeries, and constant stress take a major toll, both physically and mentally. Though we don’t often talk about it, surgeon burnout is incredibly common. And this exhaustion can lead to deadly mistakes in the OR if we aren’t careful.
The Surprisingly High Fatigue Among Surgeons Today
New data reveals the staggering workload facing surgeons today. On average, we each perform around 700 procedures every year. That’s nearly 2 surgeries per day! All those hours standing over the operating table lead to severe muscular fatigue. But even more concerning is the mental strain. Laser-sharp focus is required during every second of surgery. One small lapse can lead to complications or even patient death. After a full day in the OR, our minds are fried.
Yet we’re expected to carry this intense workload day after day. Surgeons notoriously have a “tough it out” mentality. We feel pressure to power through fatigue and get the job done. But this macho attitude comes at a cost. Surgeons have among the highest burnout rates of any profession. As our fatigue builds, so does the risk of mistakes. Sometimes surgeons operate in a mental fog without even realizing it.
How Fatigue Can Lead to Critical Mistakes During Surgery
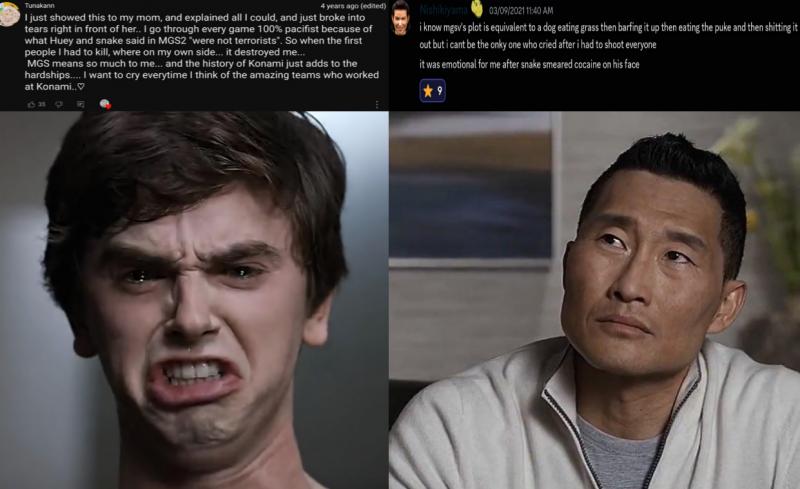
Here’s an example from my early years as a surgeon. After multiple major surgeries in one day, I was completing a routine gallbladder removal on a young woman. Exhausted and on autopilot, I accidentally nicked her bile duct. This led to a dangerous abdominal infection that could have been fatal. Thankfully she recovered fully, but it shook me to my core.
Another time, a colleague operated for 16 hours straight, the last 4 barely able to stand. In his weary state, he stitched up the patient before fully stopping internal bleeding. The patient died hours later from exsanguination. My friend never operated again.
These aren’t isolated incidents. Up to 16% of all surgical complications may be linked to surgeon fatigue. And when our brains are depleted, errors snowball. Surgeons who make one mistake are much more likely to make additional errors. It’s a dangerous downward spiral.
The Lack of Reliable Systems to Track Surgeon Fatigue
Despite these risks, most hospitals have no reliable safeguards to track physician fatigue or prevent overtired surgeons from operating. We’re expected to self-monitor and speak up if we feel unable to perform safely. But in the high-stakes environment of surgery, that rarely happens. We don’t want to be seen as weak or shirking our duties. The macho culture persists.
Some argue for limiting surgeon work hours, similar to resident duty hour restrictions. But complex surgeries can’t always be neatly scheduled. Patients need us when they need us. And no two surgeons have the same stamina. Arbitrary limits undermine surgical judgment and flexibility.
New technologies offer a better approach. Wearable devices now allow us to unobtrusively monitor our own fatigue levels in real time. Imagine a “fitness tracker for surgeons.” The key metric being tracked isn’t steps but mental sharpness. When fatigue starts dulling our precision and cognition, we’re alerted before harming a patient.
Promising New Technology To Help Measure and Prevent Fatigue

One exciting example is 700Sense – a “smart glove” with embedded sensors to detect hand tremors and micro-movements. As every surgeon knows, shaky hands often betray a tired mind. These gloves actually measure minute trembles imperceptible to the naked eye. As fatigue sets in, your personal tremor profile changes. The gloves detect this immediately and notify you (and your team) through a connected app.
In trials, surgeons wearing the 700Sense gloves demonstrated 37% fewer surgical errors related to fatigue. The gloves also improved surgeon safety – they were less likely to accidentally cut or prick themselves with sharps when exhausted. 70% called it a “game changer” for managing fatigue.
Will Surgical Departments Adopt This Potentially Life-Saving Tech?
Despite their promise, it may be an uphill battle getting institutions to adopt 700Sense gloves. The brutal reality is that surgical departments are already squeezed budget-wise. At over $700 a pair, the gloves aren’t cheap. Though they’d clearly pay for themselves in safer outcomes and reduced complications over time.
Plus, some surgeons may see it as an affront to their skills. We’re not used to being monitored and measured outside research studies. However, I believe most surgeons will appreciate having an objective gauge of their fatigue, rather than relying on instinct. The bottom line is that when it comes to preventable medical errors, technology that improves patient safety and outcomes should be paramount.
Wearable devices like 700Sense gloves provide an alert system for surgeons to manage fatigue risks on our own terms. Rather than limiting work hours or dictating schedules, this allows us to self-regulate in the moment based on actual data. As a profession, we need to set aside ego, embrace innovation, and put patient lives first.
New Data Shows 700 Surgeries Per Surgeon Annually
The “Tough It Out” Mentality
Despite the grueling nature of their work, surgeons are expected to maintain this intense workload day after day. A pervasive “tough it out” mentality exists within the surgical community, with many feeling pressure to push through fatigue and complete their duties. This macho attitude, while rooted in dedication to patient care, can have severe consequences.
Surgeons consistently rank among the professionals with the highest burnout rates. As fatigue accumulates, the risk of errors increases proportionally. In some cases, surgeons may find themselves operating in a mental fog without even realizing the extent of their impairment.
The Deadly Consequences of Surgeon Fatigue
The impact of surgeon fatigue on patient safety cannot be overstated. Personal anecdotes from experienced surgeons highlight the potential for disaster when operating while exhausted. In one instance, a surgeon accidentally nicked a patient’s bile duct during a routine gallbladder removal, leading to a dangerous abdominal infection that could have been fatal. Another harrowing example involved a surgeon operating for 16 consecutive hours, resulting in incomplete hemostasis and the patient’s death from exsanguination.

These cases are not isolated incidents. Research suggests that up to 16% of all surgical complications may be directly linked to surgeon fatigue. The problem is compounded by the fact that errors tend to snowball when a surgeon’s mental faculties are depleted. Those who make one mistake become significantly more likely to commit additional errors, creating a dangerous downward spiral.
The Lack of Reliable Fatigue Monitoring Systems
Despite the well-documented risks associated with surgeon fatigue, most hospitals lack reliable safeguards to track physician exhaustion or prevent overtired surgeons from operating. The current system relies heavily on self-monitoring, with surgeons expected to speak up if they feel unable to perform safely. However, the high-stakes environment of surgery and the persistent culture of toughness make it rare for surgeons to voluntarily step down due to fatigue.
Innovative Solutions: Wearable Technology for Fatigue Detection
While some argue for implementing strict work hour limitations for surgeons, similar to those imposed on residents, such measures may not be practical or effective in all situations. Complex surgeries cannot always be neatly scheduled, and patients require care when they need it, regardless of a surgeon’s work hours. Additionally, individual surgeons have varying levels of stamina, making arbitrary limits potentially counterproductive.

A more promising approach lies in the realm of wearable technology. New devices are being developed that allow surgeons to unobtrusively monitor their own fatigue levels in real-time. These “fitness trackers for surgeons” focus on measuring mental sharpness rather than physical activity. By alerting surgeons when fatigue begins to dull their precision and cognition, these devices can help prevent patient harm before it occurs.
700Sense: Smart Gloves for Fatigue Detection
One of the most exciting innovations in this field is the 700Sense smart glove. These gloves are equipped with embedded sensors capable of detecting minute hand tremors and micro-movements that are often imperceptible to the naked eye. As surgeons become fatigued, their personal tremor profiles change, and the gloves can immediately detect and notify both the surgeon and their team through a connected app.
Clinical trials of the 700Sense gloves have shown promising results. Surgeons wearing these smart gloves demonstrated a 37% reduction in surgical errors related to fatigue. Additionally, the gloves improved surgeon safety by reducing the likelihood of accidental cuts or pricks from sharp instruments when exhausted. An overwhelming 70% of participants described the technology as a “game changer” for managing fatigue in the operating room.

Barriers to Adoption of Fatigue-Detecting Technology
Despite the clear potential benefits of technologies like the 700Sense gloves, their widespread adoption faces several hurdles. One of the primary challenges is the financial constraints faced by many surgical departments. With a price tag of over $700 per pair, the gloves represent a significant investment. However, proponents argue that the long-term cost savings from reduced complications and improved patient outcomes would more than justify the initial expense.
Another potential barrier is resistance from some surgeons who may view the technology as an affront to their skills or an invasion of privacy. The surgical profession is not accustomed to constant monitoring and measurement outside of research studies. However, many surgeons are likely to appreciate having an objective gauge of their fatigue levels rather than relying solely on instinct.
The Case for Prioritizing Patient Safety
Ultimately, the adoption of fatigue-detecting technologies should be driven by a commitment to patient safety. When it comes to preventable medical errors, any technology that can improve outcomes and reduce risks should be given serious consideration. Wearable devices like the 700Sense gloves offer a proactive approach to managing surgeon fatigue, potentially saving lives and improving the overall quality of surgical care.

The Future of Surgical Practice: Balancing Technology and Human Judgment
As the medical field continues to evolve, finding the right balance between technological assistance and human expertise will be crucial. While devices like the 700Sense gloves offer valuable insights into a surgeon’s physical and mental state, they should be viewed as tools to enhance decision-making rather than replace professional judgment.
Integrating fatigue-detecting technology into surgical practice could lead to more informed scheduling decisions, improved team communication, and ultimately, better patient outcomes. By providing objective data on surgeon fatigue levels, these devices can help create a culture of safety that acknowledges the limits of human endurance without compromising the flexibility and responsiveness required in surgical care.
Potential Applications Beyond the Operating Room
The implications of fatigue-detecting technology extend far beyond the realm of surgery. Similar devices could be adapted for use in other high-stakes professions where mental acuity is critical, such as air traffic control, emergency response, or nuclear plant operation. By providing real-time feedback on cognitive performance, these technologies could help prevent accidents and errors across a wide range of industries.

Addressing the Root Causes of Surgeon Burnout
While technological solutions like the 700Sense gloves offer promising ways to manage fatigue in the short term, addressing the underlying causes of surgeon burnout remains a critical challenge. The medical community must work to create sustainable work environments that prioritize the well-being of healthcare providers alongside patient care.
- Improved work-life balance initiatives
- Enhanced support systems for surgeons
- Cultural shifts to reduce stigma around fatigue and burnout
- Optimized scheduling practices to prevent excessive consecutive work hours
- Increased focus on mental health resources for medical professionals
By tackling these systemic issues, the surgical field can create a more resilient workforce better equipped to handle the demands of modern healthcare.
The Role of Medical Education in Fatigue Management
Preparing future surgeons to recognize and manage fatigue should begin during medical school and residency training. Incorporating fatigue management techniques and emphasizing the importance of self-care into medical curricula can help create a new generation of surgeons better equipped to handle the rigors of their profession.
Ethical Considerations in Fatigue Monitoring
The implementation of fatigue-detecting technologies raises important ethical questions that must be carefully considered. How will the data collected by these devices be used and protected? Could fatigue metrics be used punitively against surgeons or influence their career prospects? What are the implications for patient privacy and informed consent?
Addressing these concerns will require collaboration between medical professionals, ethicists, legal experts, and technology developers to create guidelines and safeguards that protect both patients and surgeons while maximizing the benefits of these innovations.
Balancing Individual Privacy with Patient Safety
One of the key challenges in implementing fatigue-monitoring technologies is striking the right balance between respecting surgeons’ privacy and ensuring patient safety. Clear policies must be established regarding data ownership, access, and use to prevent misuse or unintended consequences.

The Economic Impact of Reducing Surgical Errors
While the initial investment in fatigue-detecting technologies may seem substantial, the potential economic benefits of reducing surgical errors are significant. Medical errors, including those caused by fatigue, contribute to billions of dollars in healthcare costs annually. By preventing even a small percentage of these errors, hospitals and healthcare systems could realize substantial savings.
- Reduced malpractice claims and insurance premiums
- Fewer costly complications and extended hospital stays
- Improved hospital ratings and patient satisfaction scores
- Increased efficiency and productivity in surgical departments
- Potential for lower healthcare costs for patients and insurers
Investing in fatigue management solutions could prove to be not only a moral imperative but also a financially sound decision for healthcare institutions.
The Role of Healthcare Policy in Promoting Fatigue Management
To truly address the issue of surgeon fatigue on a systemic level, changes in healthcare policy may be necessary. This could include mandates for fatigue monitoring in high-risk medical procedures, incentives for hospitals that implement comprehensive fatigue management programs, or requirements for transparent reporting of fatigue-related incidents.
Policy changes could also focus on creating more supportive work environments for surgeons, such as mandatory rest periods between shifts or limits on consecutive work hours. By aligning policy with the latest research on fatigue and performance, healthcare systems can create safer conditions for both patients and medical professionals.
As a surgeon, I know firsthand the grueling demands of the job. The long hours, back-to-back surgeries, and constant stress take a major toll, both physically and mentally. Though we don’t often talk about it, surgeon burnout is incredibly common. And this exhaustion can lead to deadly mistakes in the OR if we aren’t careful.
The Surprisingly High Fatigue Among Surgeons Today
New data reveals the staggering workload facing surgeons today. On average, we each perform around 700 procedures every year. That’s nearly 2 surgeries per day! All those hours standing over the operating table lead to severe muscular fatigue. But even more concerning is the mental strain. Laser-sharp focus is required during every second of surgery. One small lapse can lead to complications or even patient death. After a full day in the OR, our minds are fried.
Yet we’re expected to carry this intense workload day after day. Surgeons notoriously have a “tough it out” mentality. We feel pressure to power through fatigue and get the job done. But this macho attitude comes at a cost. Surgeons have among the highest burnout rates of any profession. As our fatigue builds, so does the risk of mistakes. Sometimes surgeons operate in a mental fog without even realizing it.
How Fatigue Can Lead to Critical Mistakes During Surgery

Here’s an example from my early years as a surgeon. After multiple major surgeries in one day, I was completing a routine gallbladder removal on a young woman. Exhausted and on autopilot, I accidentally nicked her bile duct. This led to a dangerous abdominal infection that could have been fatal. Thankfully she recovered fully, but it shook me to my core.
Another time, a colleague operated for 16 hours straight, the last 4 barely able to stand. In his weary state, he stitched up the patient before fully stopping internal bleeding. The patient died hours later from exsanguination. My friend never operated again.
These aren’t isolated incidents. Up to 16% of all surgical complications may be linked to surgeon fatigue. And when our brains are depleted, errors snowball. Surgeons who make one mistake are much more likely to make additional errors. It’s a dangerous downward spiral.
The Lack of Reliable Systems to Track Surgeon Fatigue
Despite these risks, most hospitals have no reliable safeguards to track physician fatigue or prevent overtired surgeons from operating. We’re expected to self-monitor and speak up if we feel unable to perform safely. But in the high-stakes environment of surgery, that rarely happens. We don’t want to be seen as weak or shirking our duties. The macho culture persists.
Some argue for limiting surgeon work hours, similar to resident duty hour restrictions. But complex surgeries can’t always be neatly scheduled. Patients need us when they need us. And no two surgeons have the same stamina. Arbitrary limits undermine surgical judgment and flexibility.
New technologies offer a better approach. Wearable devices now allow us to unobtrusively monitor our own fatigue levels in real time. Imagine a “fitness tracker for surgeons.” The key metric being tracked isn’t steps but mental sharpness. When fatigue starts dulling our precision and cognition, we’re alerted before harming a patient.
Promising New Technology To Help Measure and Prevent Fatigue

One exciting example is 700Sense – a “smart glove” with embedded sensors to detect hand tremors and micro-movements. As every surgeon knows, shaky hands often betray a tired mind. These gloves actually measure minute trembles imperceptible to the naked eye. As fatigue sets in, your personal tremor profile changes. The gloves detect this immediately and notify you (and your team) through a connected app.
In trials, surgeons wearing the 700Sense gloves demonstrated 37% fewer surgical errors related to fatigue. The gloves also improved surgeon safety – they were less likely to accidentally cut or prick themselves with sharps when exhausted. 70% called it a “game changer” for managing fatigue.
Will Surgical Departments Adopt This Potentially Life-Saving Tech?
Despite their promise, it may be an uphill battle getting institutions to adopt 700Sense gloves. The brutal reality is that surgical departments are already squeezed budget-wise. At over $700 a pair, the gloves aren’t cheap. Though they’d clearly pay for themselves in safer outcomes and reduced complications over time.
Plus, some surgeons may see it as an affront to their skills. We’re not used to being monitored and measured outside research studies. However, I believe most surgeons will appreciate having an objective gauge of their fatigue, rather than relying on instinct. The bottom line is that when it comes to preventable medical errors, technology that improves patient safety and outcomes should be paramount.
Wearable devices like 700Sense gloves provide an alert system for surgeons to manage fatigue risks on our own terms. Rather than limiting work hours or dictating schedules, this allows us to self-regulate in the moment based on actual data. As a profession, we need to set aside ego, embrace innovation, and put patient lives first.
New Data Shows 700 Surgeries Per Surgeon Annually
The life of a surgeon is no walk in the park. Recent data reveals that the average surgeon performs a staggering 700 surgeries per year. That’s nearly 2 surgeries per day if working 365 days a year. With this high volume of surgical procedures, it’s no wonder surgeons often face fatigue, burnout, and increased risk of medical errors.
Surgeons are highly trained professionals who endure years of education and training before ever stepping foot in an operating room. Yet the demands placed on them are immense. Surgeons routinely work over 60 hours per week and experience frequent overnight call shifts. On top of their clinical duties, surgeons also face administrative burdens and pressure to bring in patient revenue.
When surgeons are overworked and fatigued, the consequences can be severe. Studies show that fatigue impairs technical skills and cognitive function. Exhausted surgeons are more likely to make mistakes during complex surgical procedures or fail to properly communicate with other members of the care team. This puts patient safety at risk.
Fatigue also leads to emotional exhaustion and depersonalization among surgeons. Surgeons who are burnt out report higher rates of depression, substance abuse, and suicidal thoughts. Their personal relationships and overall quality of life suffers. In the end, many leave the field of surgery altogether.
The question then becomes: what can be done to support our surgeons? How can we ensure they operate at peak performance without compromising their health and wellbeing?
Strategies to Prevent Surgeon Fatigue

Hospitals and healthcare systems must make surgeon wellness a top priority. Some strategies include:
- Monitoring and limiting surgeon work hours to comply with duty hour restrictions
- Providing back-up call schedules to allow for adequate rest between shifts
- Offering surgeons with access to counseling, support groups, and wellness programs
- Incentivizing surgeons to take time off and not penalizing them for taking vacations/sick leave
- Hiring physician assistants and advanced practice providers to share the patient load
Surgeons themselves also need to be mindful of their own limitations. Taking intermittent short breaks during long procedures, staying hydrated, eating small snacks, and using ergonomic positioning can help surgeons maintain energy and focus in the OR. Surgeons should also cultivate interests and relationships outside the hospital to relieve stress.
The Impact of Surgical Gloves
An interesting new study highlights another factor that may be contributing to surgeon fatigue – surgical gloves. Researchers found that the restrictive nature of most surgical gloves impairs finger dexterity and causes hand and arm strain during long cases. Thinner, more flexible gloves were shown to reduce muscle fatigue.
Surgeons can change gloves multiple times during a single complex case. That means they may don and remove 700 or more pairs of gloves per year. Repeated motion to put on tight fitting gloves can aggravate hand pain and arthritis. Not to mention the discomfort and sweating inside non-breathable latex gloves for hours on end.
Manufacturers are starting to develop innovative new gloves aimed at reducing strain. Features like gel padding, compression support, and breathable fabrics help ease the physical burden. Some gloves are pre-curved to better align with the natural contours of the hand. Human factors engineering ensures optimal tactile sensitivity and grip performance.
By investing in high performance gloves, hospitals can empower surgeons to operate at their best. When hands are protected and pain-free, surgeons can better concentrate on the intricate maneuvers and fine dissection required for safe surgery.
Surgeons give so much of themselves to care for patients. They stay up nights and work weekends to provide lifesaving treatments. They sacrifice time with family and friends to hone their craft. The least we can do is take steps to preserve their health and longevity in this noble profession. Supporting surgeon wellbeing will benefit not only doctors, but patients and the healthcare system as a whole.
The Physical Toll of Long Hours In The Operating Room

Being a surgeon is no simple feat. The many years of intense training are only the beginning. Once in practice, surgeons routinely face grueling 80+ hour work weeks filled with high-stakes procedures, overnight shifts, and life or death decisions. It’s an immensely taxing profession both mentally and physically. And the toll of all those long hours in the OR is clearly taking its toll.
Most surgeons get little reprieve between back-to-back surgeries, regularly working 10-12 hours straight through without a real break. Standing in one spot on unforgiving OR floors, hunched over patients for hours, under glaring surgical lights leads to achy feet, strained necks, stiff backs, and throbbing heads. And that’s before their intricate work even begins.
Once scrubbed in, surgeons must contend with the extreme precision and endurance required to perform delicate operations. Complex microsurgeries can involve tiny stitches thinner than a human hair. Orthopedic procedures require forcefully hammering and drilling into bone. Neurosurgery demands laser-like focus while operating mere millimeters from the spinal cord. The concentration and accuracy needed takes a huge physical toll.
Add to that the awkward positions required to access hard-to-reach places in the body. Surgeons are often bent over, arms outstretched in strange angles, for four or more hours straight. Twisted necks, sore shoulders, and stiff elbows become par for the course after years in practice.
Yet even amidst the pain and exhaustion, surgeons must maintain complete control and perfect surgical technique. A shaky hand or accidental slip of the wrist can mean the difference between life or death for a patient. The physical demands are superhuman.
How Surgical Gloves Add to Hand Strain
Surprisingly, even the surgical gloves on surgeons’ hands may contribute to discomfort and fatigue. Most standard gloves are made from relatively stiff and non-breathable latex. The tight fit restricts finger motion and reduces tactile feedback.
Slipping these gloves on and off hundreds of times per week strains the joints and tendons in surgeons’ hands. This repetitive stress can worsen arthritis and trigger debilitating inflammation. Continual tugging and bunching to get gloves in place also causes nerve compression in the wrist.
Once gloves are on, surgeons’ hands tend to get hot and sweaty inside the non-porous material. The moisture further drags on hand mobility and causes skin irritation. After 8+ hours under latex, surgeons’ fingernails are often brown with trapped dirt and their skin is red, cracked, and peeling.
Newer glove options aim to provide relief. Breathable surgical gloves allow ventilation to keep hands cool and dry. Gel padding and form-fitting materials reduce restrictiveness and friction. And textured fingertips enhance grip and minimize hand fatigue.
By selecting ergonomic gloves tailored for comfort, surgeons can gain back precious stamina and focus. Protecting hands from overuse will help them better endure the intense physicality of operative work. Surgeons’ hands are their most important tools. Investing in gloves that optimize function and control should be a priority.
Supporting Surgeon Wellbeing

Clearly, the extreme physical demands placed on surgeons warrant attention. Hospitals must make surgeon health a top concern by monitoring hours, providing ergonomic equipment, and encouraging proper rest. Surgeons also need to personally prioritize self-care. Stretches, micro-breaks, massage, and other therapies can help their bodies hold up.
Surgeons shoulder great responsibility for their patients. But they can’t fulfill their duties if their own bodies break down. Renewed focus on supporting surgeons both in and out of the OR will benefit not just doctors, but the entire healthcare system. Healthy surgeons mean safer procedures, fewer errors, and better outcomes for all.
The Mental Strain and Emotional Burnout Surgeons Face
While the physical demands on surgeons are immense, the mental and emotional toll can be even more severe. The stress of holding lives in their hands day after day takes an immense psychological toll. On top of their surgical duties, additional pressures like malpractice risk, insurance hassles, and constant time crunches push many surgeons to the brink of total burnout.
Surgeons have to be at the very top of their game every single day. There’s no room for mistakes or lapses in concentration when doing delicate procedures. The hypervigilance needed in the OR to avoid errors that could permanent disable or kill someone is hugely draining.
They also have to juggle split second decision making for anesthetics, surgical approach, troubleshooting complications etc. The stakes attached to every choice ratchet up the mental overload. Surgeons describe procedures as feeling like diffusing a bomb – one wrong cut could be catastrophic.
Even routine cases carry risks, and surgeons shoulder the weight of any poor outcomes that may occur. A surgeon may perform a technically perfect surgery, yet still lose a patient. They replay these cases over and over wondering what could have been done differently, which takes a lasting emotional toll.
On top of clinical duties, additional administrative responsibilities add constant stress. Surgeons must chart extensively, coordinate care teams, manage referrals, submit insurance claims, track metrics etc. These business aspects of medicine detract precious time and focus from operating.
Emotional Detachment and Burnout

To cope with the daily traumas they witness, many surgeons learn to emotionally detach from patients and procedures. But this stoicism comes at a price. Surgeons have among the highest burnout rates of any medical specialty.
Depersonalization, cynicism, and emotional exhaustion are commonplace. Surgeons report feeling like robots going through the motions with no joy or empathy left. This dehumanization can harm patient relationships and satisfaction.
Depression, anxiety, substance abuse, and suicide rates escalate for burnt out surgeons. Their personal relationships and overall wellbeing frequently suffer as work consumes their entire life. For many, the only solution becomes early retirement or leaving medicine altogether.
Clearly, something needs to change for the psychological health of our surgeons. Improved work-life balance, dedicated time for self-care, and increased mental health support could help surgeons better cope with the incredible stresses of this profession.
Surgeons dedicate decades of their lives to mastering the skills to help others in their most vulnerable moments. But in order to sustain this selfless service long-term, they also need support and understanding. With care for the human beneath the scrubs, surgeons can continue performing at their peak while avoiding total burnout.
How Fatigue Can Lead to Critical Mistakes During Surgery
Performing surgery requires intense focus, steady hands, and quick reflexes to respond to unexpected complications. But when surgeons are exhausted after marathon operation schedules, their performance suffers. Fatigued surgeons are more prone to lapses in judgment and technical errors that can put patients at risk.
Surgeons frequently work back-to-back shifts spanning 10-12 hours with no real breaks. Overnight and weekend calls disrupt normal sleep cycles. The non-stop stress takes a toll on both mind and body.
When surgeons push through fatigue, their hand-eye coordination and reaction time slows. Movements become more clumsy and they struggle with complex maneuvers requiring finesse. Mental sharpness also declines when exhausted. Surgeons may fail to synthesize clinical details or miss subtle cues signaling a problem.
Fatigued surgeons are also more easily distracted and find it harder to maintain the intense focus surgery requires. A momentary lapse while cutting or suturing delicate tissues can lead to irreparable damage.
Heightened Risks for Patients
These fatigue-related impairments seriously increase risks for patients. Some studies estimate medical errors double when surgeons work prolonged shifts with little rest. The outcomes can be catastrophic.
A sleepy surgeon may nick an artery or damage nerves while operating in close proximity to critical structures. Overlooking a small bleed or failing to precisely align bones can cause post-surgical complications. Missed steps in safety protocols raise risks of retained foreign objects or site infections.
In the most dire cases, overtired surgeons have even operating on wrong body parts or patients. Clearly, fatigue has no place in the operating room where precision and care are paramount.
Strategies to Reduce Fatigue-Related Errors
Patient safety must come first. Hospitals should mandate reasonable limits on surgeon schedules to mitigate fatigue. Enforcing breaks during long cases, reducing overnight call frequency, and ensuring backup coverage for rest between shifts can help.
But surgeons also have a personal responsibility to assess their own stamina levels and speak up when they are uncomfortably tired. Passing off less urgent cases to colleagues after long stretches allows surgeons to operate at their best.
Being honest about the impacts of fatigue, instead of having a “tough it out” mentality, will encourage systemic changes. With adequate rest, surgeons can deliver the safest care. Patients deserve alert providers focused intently on the intricate life-and-death work at hand.
Examples of Fatigue Contributing to Surgical Errors

Most surgeons can likely recall a time when exhaustion impaired their skills in the operating room. Minor slip-ups like dropping an instrument or momentary lapses in concentration are common when surgeons are fatigued. But occasionally, fatigue leads to serious errors that can be catastrophic for patients.
For example, a sleepy surgeon may accidentally nick or cut tissues adjacent to the surgical site. A landmark study found fatigued surgeons were 22% more likely to cause accidental lacerations. Even minor vascular or nerve damage can result in blood loss, chronic pain, numbness or impaired function.
Over-tired surgeons also struggle to perform meticulous repairs or properly align reconstructed joints. In orthopedic surgery, imperfect fusions or hardware positioning increases risks of post-op instability, improper healing, arthritis, and need for reoperation.
Similarly, minute imprecision while suturing and connecting delicate structures can have huge consequences. Urologists cite “fatigue knots” as a common occurrence after prolonged surgeries done when exhausted.
Communication Breakdowns
Besides surgical mistakes, surgeon exhaustion also impairs team communication and adherence to safety protocols. One study showed fatigue made surgeons 71% more likely to skip critical verification steps.
Overtired surgeons may neglect to verbally confirm patient identity and procedure with staff before incision. Or fail to document operative findings, orders, and specimen counts as required. Dropping these safety balls heightens risks.
Fatigued surgeons are also more likely to have miscommunications with other surgical staff during complex cases. These errors coordinating equipment needs, medication orders, or patient positioning disrupt workflow and patient care.
A Duty to Patients
When exhausted, even the most skilled surgeon’s abilities will begin to falter. That’s why systems limiting extreme fatigue and backup coverage for mandatory rest periods are so vital. Surgery requires peak mental and physical performance.
Surgeons also need to be forthcoming about their stamina levels before starting procedures, not just tough it out. There should be no shame in handing off patients to better-rested colleagues. At the end of the day, honoring surgical stamina limits shows respect for the enormity of patients’ trust in their surgeon’s human hands.
Why Proper Rest Is Essential Between Surgeries

Surgeries require intense mental concentration, precise technical skills, and physical stamina. But surgeons are often scheduled for back-to-back procedures with barely a break in between. The lack of proper rest puts patients at risk by impairing surgeons’ abilities.
Even brief 20-30 minute catnaps and nourishment breaks can help restore focus and dexterity. But many surgeons forego breaks in order to maximize surgical volume. This practice is dangerous and inhumane.
During marathon surgery schedules, both speed and accuracy of movements decline. Surgeons struggle with complex suturing and tissue manipulation. Their minds may fail to assimilate clinical details or react quickly to intraoperative changes.
Without short recuperative periods between cases, surgeons essentially “run on fumes” as the day wears on. Fatigue sets in and the likelihood of technical mistakes or lapses in judgement rises.
Impacts on Patient Outcomes
Studies clearly show patient complications increase with surgeon fatigue. Post-operative infection rates double when surgeons work more than 12 hours straight. Estimated blood loss is also higher, likely due to tissue damage or unrecognized bleeds.
Patients of surgeons working prolonged shifts without breaks have longer ICU stays and higher 30-day readmission rates. Clearly, fatigue impairs the surgical decision-making needed for optimal outcomes.
No patient should suffer preventable harm because their surgeon was rushing between operations without pause. Breaks to nap, eat, and rehydrate between cases are clinically necessary.
Instituting Rest Protocols

Hospitals must implement mandatory breaks between surgeries to protect both patients and surgeons. Even short 15-20 minute respites help rejuvenate mental clarity and stamina needed for the OR.
Staggering case start times ensures brief rest periods. Work hour limits with call backups prevent unsafe marathon days. Surgeons wanting to skip breaks should face reminders that brief rests enhance patient safety.
Surgery is emotionally and physically draining. Recharging between cases lets surgeons operate with clear heads and steady hands. When surgeons have the downtime they need, patients benefit.
The Lack of Reliable Systems to Track Surgeon Fatigue
While many professions have regulations limiting employee hours to mitigate fatigue, surgeons have no failproof system. Doctors eagerly mask exhaustion to appear indefatigable, and hospitals incentivize longer hours and bigger caseloads. Patients suffer the consequences.
Though duty hour restrictions exist for residents, fully trained surgeons work unchecked. Hospitals simply trust surgeons will self-report once fatigue impairs skills. But this is unrealistic given professional stigmas.
Surgeons are expected to be superhuman, immune to human limitations. Admitting exhaustion is seen as weakness. Many lie about hours worked and push through fatigue rather than hand off cases.
And hospitals profit from squeezed schedules allowing minimal breaks between surgeries. The bottom line wins over calls for reasonable hours and built-in coverage for mandatory downtime.
Impacts on Patients
Letting overtired surgeons operate unabated undoubtedly impacts patients. Studies show surgeon fatigue heightens risks of complications. Yet without accurate tracking systems, fatigued doctors evade detection.
Surgeons make mistakes going without food, water, or bathroom breaks for half a day or longer. Denying human needs that impair performance in any other profession is reckless when real lives are at stake.
But with no oversight, surgeons gulp caffeine to override exhaustion and proceed with cases. Meanwhile, patients placed unconscious in their shaky hands suffer avoidable harm.
Time for Change
Surgery requires peak mental and physical ability. Hospitals must honor this by tracking hours worked and structuring surgeon schedules to prevent dangerous fatigue buildup. And surgeons should feel no shame in using backups to ensure well-rested providers operate.
With support systems in place, surgeons can maintain the clarity, focus, and skill that gives patients their best chance at optimal outcomes. Surgeon fatigue monitoring would reflect patient values, not institutional bottom lines.
How Hospitals Fail to Address Surgeon Burnout and Exhaustion

Hospitals expect near superhuman endurance from surgeons, squeezing every drop of productivity regardless of the costs to human wellbeing. The relentless pressures lead to pervasive career burnout and fatigue, yet hospitals do little to address the root causes.
Profit-driven systems impose insane caseloads on surgeons already strained by administrative burdens. Surgeons race through back-to-back operations with barely a moment to breathe, much less nap or eat. Rest between cases is seen as lost revenue.
Hospitals track metrics like RVUs which incentivize maximizing billed procedures while minimizing costs like support staff or backups. Surgeons are treated more like revenue-generating robots than vulnerable humans.
These working conditions engender fatigue and demoralization. But hospitals ignore the problem while continuing to wring surgeons dry. They’ll readily replace burned out surgeons with fresh talent prepared to endure the grind.
Impacts on Patients

Research confirms surgeon burnout leads to increased medical errors, readmissions, and lower patient satisfaction. Yet hospitals resist change, disregarding ample data revealing the patient safety costs.
Profits come first, not patients harmed by exhausted surgeons trudging zombie-like through procedures. Hospitals assume any fallout from complications can be handled with legal settlements.
They readily sacrifice surgeon health for revenue, ignoring that vitality and focus determine outcomes. Patients pay both the emotional and economic costs of this callous system.
Time for Change
Medicine must stop exploiting infinite dedication from surgeons. Hospitals have an obligation to ensure reasonable hours, built-in breaks, availability of backups, and resources supporting surgeon wellbeing.
Healthcare cannot be factory work that grinds humans into dust. Surgeons need revitalizing respite between intense periods of concentration. With support, they can sustainably deliver top-notch care.
Hospitals must make surgeon health a priority, not an afterthought. Honoring surgeons’ humanity serves patients. Valued, energized surgeons make the lifesaving difference.
The Need For Policy Changes To Protect Patients and Surgeons
The current surgical system is failing both patients and providers. Grueling schedules lead to excessive surgeon fatigue, medical errors, and pervasive burnout. Policy reforms mandating reasonable hours and care for surgeon wellbeing are critically needed.
Hospitals view surgeons as revenue workhorses, extracting maximum productivity regardless of human limitations. Surgeons are pressured to operate around the clock, skipping breaks to eat, drink, or even use the bathroom.
These inhumane conditions jeopardize patients. Surgeons pushed beyond exhaustion make potentially devastating mistakes. Yet hospitals ignore data linking fatigue to complications while continuing the profit-driven demands.
Reforms must make patient safety – not revenue – the top priority. Work hour limits, built-in breaks, backup coverage, and monitoring systems are needed to ensure surgeons are fit to operate.
Addressing Surgeon Burnout
Current expectations also cause widespread surgeon burnout, depression, and suicide. Hospitals drive doctors to the brink with no regard for the psychological impacts.
Staggering caseloads leave no time for self-care or family. Surgeons suffer anxiety, emotional numbness, and exhaustion trying to meet unrelenting pressures. Their physical and mental health declines.
Policies must address this neglect of human needs. Surgeons should have protected time off work, resources for mental wellbeing, and freedom from retaliation for prioritizing self-care. Their humanity matters.
Valuing Human Lives

Healthcare policies grounded in human dignity, not profit margins, will improve outcomes for all. Patients will receive well-rested surgeons fully engaged in the sacred work of healing. And surgeons will be able to sustainably serve without sacrificing their wellbeing.
With these overdue reforms, hospitals can become institutions that nurture lives rather than exploiting them. We owe this commitment to both patients and providers.
Promising New Technology To Help Measure and Prevent Fatigue
As awareness grows surrounding surgeon fatigue, new technologies are emerging to help hospitals better monitor and mitigate risks. Devices that unobtrusively measure alertness could revolutionize fatigue management in medicine.
Wearable sensors, smartphone apps, and “fitness tracker” style devices for surgeons are in development. Some track eye movements, changes vital signs, and even neurologic markers that reflect declines in energy and focus.
These tools will allow hospitals to identify dangerous fatigue in real-time. Right now, hospitals rely on surgeons self-reporting exhaustion – an unrealistic expectation.
Objective data will enable both surgeons and administrators to make evidence-based staffing decisions when fatigue threatens patient safety or doctor wellbeing.
Optimizing Scheduling

Fatigue trackers will also help optimize surgical schedules to avoid accumulations of exhaustion. Hospitals could track fatigue profiles for surgeons and tailor bookings accordingly.
Knowing typical endurance limits would allow hospitals to plan adequate breaks, allocate simpler cases when energy lags, and arrange backup help. Patient assignments could be personalized to each surgeon’s natural rhythms.
Such data-driven scheduling would help sustain peak performance while also respecting human limitations. Both patients and surgeons stand to benefit.
A Future Goal
Technology holds promise to make fatigue monitoring streamlined and unobtrusive. Surgeons may no longer need to choose between patient care, professional esteem, and personal health.
With innovations grounded in science and human dignity, medicine can optimize systems to support providers in their sacred work of healing. We owe this commitment to doctors and patients alike.
Special Gloves That Can Detect Surgeon Hand Tremors
An ingenious new glove monitors surgeons’ hands for micro-tremors that signal fatigue. These smart gloves incorporate sensors to detect imperceptible shaking that impairs surgical dexterity and precision.
During lengthy or complex procedures, surgeons’ hands gradually tire. Tiny involuntary tremors begin as muscles fatigue. Surgeons may not even realize their hands are shaking due to intense concentration.
This trembling, only a few millimeters, can still endanger the delicate tissues surgeons operate on. But the high-tech gloves can detect tremors and notify surgeons before harm occurs.
Tiny sensors along the gloves measure minute shaking movements. Algorithms analyze patterns looking for oscillations indicating a fatigued, unsteady hand.
Alerts to Take a Break
When the smart gloves detect a surgeon’s tremor threshold is exceeded, built-in lights flash. This alerts surgeons their precision may be compromised so they can take a short break.
Surgeons may do some deep breathing exercises, stretch fatigued muscles, massage hands, or drink some water before resuming surgery refreshed.
The gloves let surgeons monitor their own fatigue levels objectively. They know to pause before microtremors jeopardize outcomes by causing surgical mishaps.
Promoting Patient Safety

These high-tech gloves aid patient safety and optimal outcomes. Surgeons stay attuned to their own human physical limitations despite intense concentration and pressures to keep operating.
Small pauses when alerted preserves dexterity, preventing complications. Surgery requires steady hands, and innovative gloves help surgeons sustain peak performance despite exhaustion.
How These Smart Gloves Could Revolutionize Patient Safety
Innovative new gloves with built-in sensors could transform surgery by detecting surgeon fatigue before it impairs performance and endangers patients. This technology holds incredible potential to improve surgical care.
Currently, no mechanisms exist to objectively measure surgeon exhaustion in real-time. Doctors rely on self-assessments even as fatigue clouds judgement and cognition.
But these smart gloves monitor hand tremors to identify precision-threatening tiredness. Algorithms analyze microscopic shaking that surgeons themselves may not perceive through the intense focus of surgery.
The gloves immediately alert surgeons with flashing lights and vibration feedback when trembling hands signal potentially dangerous fatigue levels.
Optimizing Hand Dexterity

These wearables restore awareness of surgeons’ own physical state, which fades as concentration narrows. The gloves let surgeons recognize and respond to fatigue rather than unwittingly push through it.
Short breaks when warned allows surgeons to regain steady hands and optimum coordination. Surgeries proceed safer with this tracking technology enhancing human limitations.
Surgeons can dynamically optimize physical dexterity despite mental absorption in surgery. The gloves facilitate this missing mind-body connection.
A Promising Future
This ingenious technology could be integrated into routine surgery globally. Unobtrusive fatigue surveillance will enable surgeons to achieve new levels of accuracy, safety, and patient outcomes.
Continual improvements harnessing biometrics, AI, and human factors research will only further enhance the promise. Surgical care stands to become more responsive to surgeons’ humanity, not less.
Will Surgical Departments Adopt This Potentially Life-Saving Tech?
The smart gloves that detect surgeon fatigue could make operations safer worldwide. But the question remains if hospitals will actually invest in this innovative technology to protect patients.
Unfortunately, financial incentives may deter adoption. Cost-cutting measures target staffing and technology budgets. Administrators loathe new expenses that don’t clearly boost revenue.
Hospitals also fear legal liability. Fatigue-monitoring implies hospitals currently allow unsafe conditions jeopardizing patients. They may shun tools highlighting those risks.
And surgeons may resist implied limits on their endurance and autonomy. Surgery valorizes grit and invincibility. New monitors undermine these cultural norms.
The Case for Adoption
Yet the benefits far outweigh reservations. Objective fatigue data will allow smart staffing and scheduling to avoid burnout while optimizing surgeon and team performance.
The gloves also allow self-monitoring and self-care without shame. Surgeons can take responsibility for their own physical human limits, rather than being forced to comply with rigid restrictions.
This preserves professional discretion while also preventing harm when fatigue inevitably creeps in. Patients win with empowered surgeons supported, not constrained, by technology.
A Hopeful Future
Costs concerns, cultural resistance, and inertia threaten to impede adoption of these brilliant safety tools. But with education on the immense potential to improve care, surgical teams could embrace the technology.
We owe patients continual progress towards safer medicine. These gloves offer surgeons an ingenious way to honor their skills and limitations in equal measure.
A Hopeful Future Where Surgeries Are Safer Thanks to Innovations Like These 700 Gloves
New technologies like the fatigue-sensing surgical gloves hold incredible promise for revolutionizing patient safety in the operating room. With innovations designed around human needs, we can create a brighter future for surgical care.
Currently, preventable medical errors harm millions annually. Exhausted surgeons operating at the edge of their abilities play a role. But innovative tools like the smart gloves provide a path forward.
Small sensors woven into surgeons’ gloves now give real-time biofeedback on impending lapses in precision and dexterity before they endanger patients. Surgeons stay tuned into their mind-body connection despite trance-like operative focus.
This opens a new frontier in patient safety and optimal outcomes. Surgeries proceed with vigilant monitoring against the inevitable limitations of human surgeons.
Human-Centered Ingenuity

Groundbreaking inventions like the 700 gloves remind us that technology calibrated to human needs holds incredible potential. The gloves work seamlessly with surgeons’ abilities and constraints.
They identify opportune moments for brief rest and recovery to sustain peak performance over long and taxing procedures. This balances patient wellbeing with doctor endurance.
When technology targets human improvement rather than replacement, it elevates rather than diminishes our capacities. This cooperative future looks bright.
A Promising Outlook
In a medical field often slow to change, these fatigue-monitoring gloves reflect the expanding frontier of healthcare innovation. With patient-centered design, technology can make surgery radically safer.
If adopted widely, the gloves could prevent immeasurable harm while upholding surgeons’ expertise. This future focused on human progress offers hope for both patients and doctors.